SMi Source lesson Asthma: MOA has the following microlearning topics
1. Inhaled Corticosteroids (ICS)

2. Leukotriene Modifiers

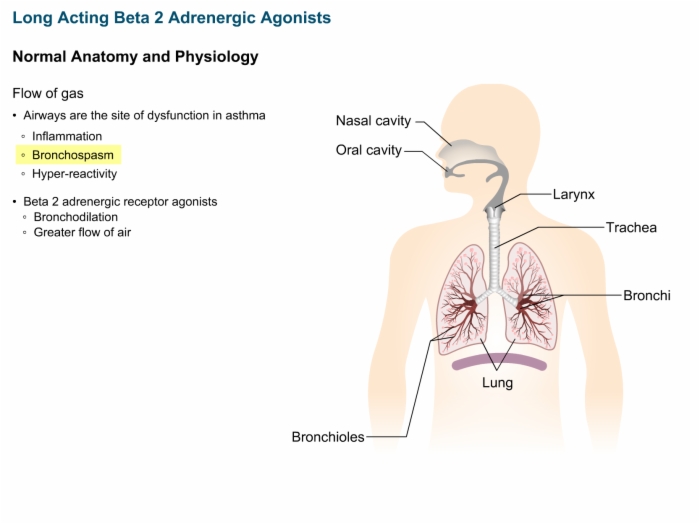
3. Long-Acting Beta 2 Adrenergic Agonists

Lesson Asthma: MOA teaches these concepts
Asthma, Inhaled Corticosteroids (ICS), Important Features of Corticosteroid Therapy in the Treatment of Asthma
Asthma, Inhaled Corticosteroids (ICS), Corticosteroids: Cellular Mechanisms of Action
Asthma, Inhaled Corticosteroids (ICS), Corticosteroids: Molecular Mechanisms of Action
Asthma, Inhaled Corticosteroids (ICS), Corticosteroids
Asthma, Inhaled Corticosteroids (ICS), Normal Respiration
Asthma, Inhaled Corticosteroids (ICS), How Does Asthma Affect Respiration?
Asthma, Inhaled Corticosteroids (ICS), Corticosteroid Mechanism of Action
Lesson Asthma: MOA addresses these key points
Local delivery of inhaled corticosteroids:
- Puts a minimal amount of corticosteroids into the rest of the body (systemic bioavailability)
- Side effects:
- Oral candidiasis
- Hoarseness
- Cough
Factors that effect local versus systemic bioavailability of inhaled corticosteroids:
- Onsite activation
- Oral bioavailability
- Protein binding
- Receptor affinity
Local vs. systemic effects:
- Fraction of dose deposited within the mouth and pharynx upon administration:
- Rinsed out or swallowed
- First pass inactivation or systemic circulation
- Drug particle size
- Fraction of dose deposited in the lung upon administration:
- Receptor binding affinity
- Half-life
- On-site activation
- Plasma protein binding
Corticosteroids:
- Reduce leukocyte chemotaxis
- Decrease vascular permeability
- Promote apoptosis of eosinophils
- Reduce mucus production
- Increase beta 2 adrenergic receptor numbers and bronchodilation
Lipocortin:
- Produced as one of the cellular actions of glucocorticoids
- Inhibits the enzyme phospholipase A2 which is responsible for the synthesis of arachidonic acid
Arachidonic acid:
- Precursor for:
- Eicosanoids or prostaglandins
- Leukotrienes
In asthma there is increased production and release of eicosanoids during degranulation, which contributes to airway inflammation.
Inhaled corticosteroids:
- Act to prevent:
- Eicosanoid-induced airway constriction
- Infiltration of white blood cells
- Vascular permeability
- Inflammation in response to these factors
Cyclooxygenase:
- Enzyme that converts arachidonic acid into prostaglandins
- Two isoforms:
- COX1
- COX2
- Expression of COX2 is inducible and increased dramatically by inflammatory cytokines
- Corticosteroids inhibit the upregulation of COX2 in response to these cytokines
Inhaled corticosteroids:
- Potent anti-inflammatory agents
- Mainstay of long-term control of airway inflammation
- First line controller therapy for persistent asthma
- Improve patient outcomes
- Reduce medical care cost and use of resources
Bronchial tubes:
- Outer walls are surrounded by smooth muscle that contracts and relaxes in response to chemical and neuronal stimulation
- Inner lining (bronchial mucosa) contains mucus glands and inflammatory cells
Inflammatory cells:
- Protect the bronchial mucosa from inhaled microorganisms and allergens
- Important players in the allergic reaction
- Prime therapeutic targets in asthma
Asthma:
- Narrowing of the respiratory airways
- Restricts the movement of air in to and out of the lungs
- Caused by three major factors:
- Inflammation
- Bronchospasm
- Hyper-reactivity
Inflammation:
- Most important factor causing narrowing of the bronchial tubes
- Occurs in response to allergen and/or irritant exposure
Bronchospasm:
- Caused by substances released by mast cells or eosinophils undergoing degranulation after allergen binds to IgE receptors
- Also caused by acetylcholine-releasing neurons after being stimulated during activation of irritant receptors in response to histamine and other factors
Prolonged inflammation in asthma:
- Induces a state of airway hyper-reactivity to irritants, allergens, and agents causing bronchoconstriction
- Can lead to permanent reduction in the size of the airways
Glucocorticoids:
- Steroid hormones
- Decrease the synthesis of inflammatory cytokines by white blood cells and bronchial epithelial cells
Corticosteroid mechanism of action:
- Glucocorticoids pass through the plasma membrane of the cell into the cytoplasm where they bind to intracellular glucocorticoid receptors
- The receptors dimerize and enter the nucleus
- In the nucleus, the glucocorticoid-receptor complex binds to specific regions of DNA to effect gene transcription and synthesis of proteins that affect cellular function
Lesson Asthma: MOA is built from these main references. Log into SMi Source for a complete list and details.
L.-P. Boulet. Once-Daily Inhaled Corticosteroids for the Treatment of Asthma. Curr Opin Pulm Med. 10(1):15-21, 2004.
H. Derendorf, R. Nave, A. Drollman, F. Cerasoli, W. Wurst. Relevance of Pharmacokinetics and Pharmacodynamics of Inhaled Corticosteroids to Asthma. Eur Respir J. 28:1042-1050, 2006.
J.G. Fernandez-Morata, J. Mollol, M. Fuentes, L. Pujols, J. Roca-Ferrer, M. Perez, A. Xaubet, C. Picado. Regulation of Cyclooxygenase-1 and -2 Expression in Human Nasal Mucosa: Effects of Cytokines and Dexamethasone. Clin Exp Allergy. 30(9):1275-1284, 2000.
J.W. Georgitis. The 1997 Asthma Management Guidelines and Therapeutic Issues Relating to the Treatment of Asthma. Chest. 115:210-217, 1999.
M.T. Halpern, Z.M. Zhan, H. Stanford, K.M. Spayde, M. Golubiewski. Asthma: Resource Use and Costs for Inhaled Corticosteroid vs Leukotriene Modifier Treatment—A Meta-Analysis. 52(5):382-389, 2003.
J.C. Mak, T. Hisada, M. Salmon, P.J. Barnes, K.F. Chung. Br J Pharmacol. Glucocorticoids Reverse IL-1β-Induced Impairment of β-Adrenoceptor-Mediated Relaxation and Up-Regulation of G-Protein-Coupled Receptor Kinases. 135(4):987-996, 2002.
T. Nittoh, H. Fujimori, Y. Kozumi, K. Ishihara, S. Mue, K. Ohuchi. Effects of Glucocorticoids on Apoptosis of Infiltrated Eosinophils and Neutrophils in Rats. Eur J. Pharmacol. 354(1):73-81, 1998.
L. Sautebin, R. Carnuccio, A. Ialenti, M. Di Rosa. Lipocortin and Vasocortin: Two Species of Anti-Inflammatory Proteins Mimicking the Effects of Glucocorticoids. Pharmacol Res. 25(1):1-12, 1992.
R.P. Schleimer, B.S. Bochner. The Effects of Glucocorticoids on Human Eosinophils. J. Allergy Clin Immunol. 94(6 pt 2):1202-1213, 1994.
A.P Wright, J. Zilliacus, I.J. McEwan, K. Dahlman-Wright, T. Almlof, J. Carlstedt-Duke, J.A. Gustafsson. Structure and Function of the Glucocorticoid Receptor. J Steroid Biochem Mol Biol. 47(1-6):11-19, 1993.
Lesson Asthma: MOA introduces and defines these terms
Chemotaxis: Movement of cells toward chemical signals.
Apoptosis: Programmed cell death.